Comprehensive Oral Surgery Care, Jacksonville, FL
In addition to Corrective Jaw Surgery and Facial Cosmetic Surgery, we offer all aspects of Oral Surgery including:
• The removal of Wisdom teeth
• Exposure of Impacted Teeth for Orthodontics
• Placement of Dental Implants
• Bone Grafting to the Jaws and Facial Bones
• Treatment of Pathologic Lesions of the Face, Mouth, and Jaws
• Treatment of Injuries of the Face, Mouth, and Jaws
Our goal is to provide our patients with the highest level of oral surgery care in a safe and caring environment. We provide our patients with the latest technology and techniques provided by an experienced surgeon and supported by a staff of experienced, caring professionals. Our office is equipped with the newest digital Xray equipment including CBCT (Cone Beam CT Scan) for precise placement of dental implants and planning of Orthognathic surgery.
Wisdom Teeth
What are wisdom teeth?
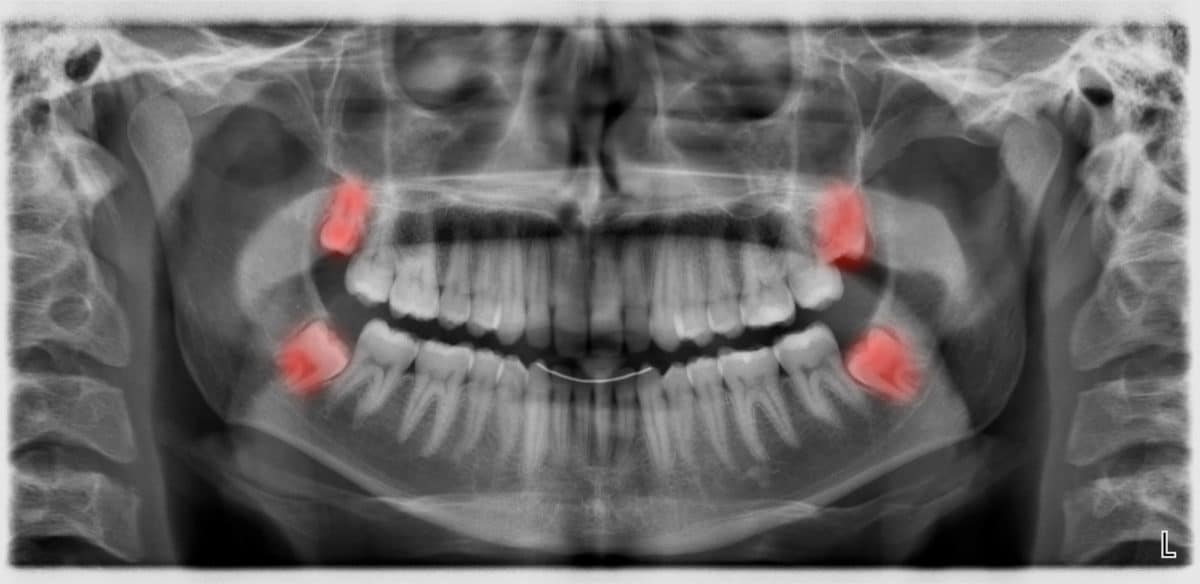
Third molars are commonly referred to as wisdom teeth. They are usually the last teeth to develop and are located in the back of your mouth, behind your second molars. Their development is usually completed between the middle teenage years and early twenties, a time traditionally associated with the onset of maturity and the attainment of wisdom.
What is an impacted tooth?
Although most people develop and grow 32 permanent adult teeth, many times their jaws are too small to accommodate the four wisdom teeth. When inadequate space prevents the teeth from erupting they are called impacted wisdom teeth. This indicates their inability to erupt into the proper position for chewing and cleaning.
We will need to see you for a consultation to determine if you will benefit from wisdom tooth removal. A special x-ray of your mouth and jaws (panorex) will be taken to determine if your wisdom teeth are impacted, or if there is room for them to erupt, and how difficult it will be to have them removed.
Wisdom Teeth Removal
Consultation and Oral Surgery Examination
Dr. Richard Joseph will evaluate the position of the wisdom teeth with an oral surgery examination and x-rays of the mouth. He can advise you if there are present or future potential problems. Studies show that early evaluation and treatment result in a better outcome for the patient. Patients are generally first evaluated in the mid-teenage years by their dentist, orthodontist, or by an oral and maxillofacial surgeon.
Why should I have my wisdom teeth removed?
If you do not have enough room in your mouth for your third molars to fully erupt, a number of problems can happen. Impacted Wisdom teeth should be removed before their root structure is fully developed. In some patients, it is as early as 12 or 13, and in others, it may not be until the early twenties. Problems tend to occur with increasing frequency after the age of 30. Some of the possible problems related to not removing your wisdom teeth include:
• Infection
• Cyst Formation
• Crowding
• Damage to Adjacent Teeth
What happens on the day wisdom teeth are removed?
Your outpatient oral surgery is performed under appropriate anesthesia to maximize your comfort. You will be given Anesthesia Options at your consultation. Most people prefer to be sedated when they have their wisdom teeth removed. We utilize modern monitoring equipment and our staff has the training, and experience to provide various types of anesthesia in a safe environment. Our oral surgery team, the office facilities, and the doctor are inspected and licensed by the State of Florida on a regular basis.
A parent or responsible adult should accompany you to the office and plan to stay with you the rest of the day. The procedure will take about 30 to 60 minutes and you will probably be in the office for 90 minutes. State-of-the-art sterilization and infection control techniques are used at all times.
On the morning of your oral surgery, it is essential that you have nothing to eat or drink (except prescribed medications with a sip of water) for at least 6 hours. Having anything in your stomach increases the risk for serious anesthetic complications, including nausea and vomiting. We may provide you with a prescription for pain medication at your consultation appointment, which can be filled in advance.
If you are going to be sedated, we will place an IV in your arm. This is a quick and nearly painless procedure that ensures optimal delivery of your medication. Another option includes the use of oral sedation or a sleeping pill. Local anesthesia is then given to ensure comfort. You will be sleepy for a significant portion of the day.
If your oral surgery requires stitches, these usually dissolve in 3 to 5 days and do not require removal. You may also experience swelling. This is all part of the normal recovery and will subside in several days.
Most patients will return for a follow-up visit usually 7-10 days later.
Dental Implants
What are dental implants?
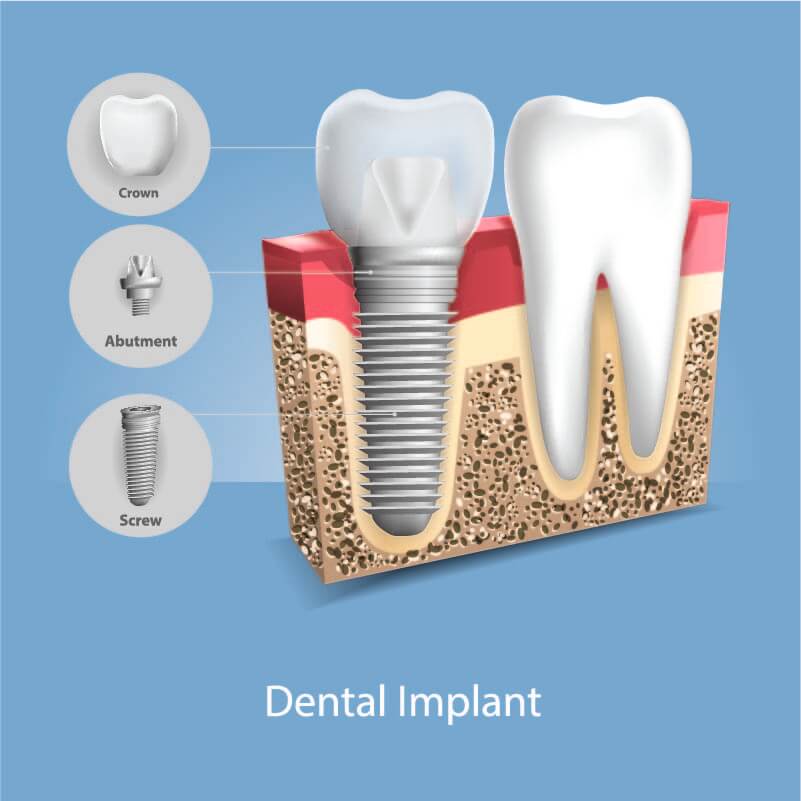
A natural tooth consists of a root and a crown. Dental implants made of titanium replace the root under the gum and are anchored into the jaw. They also have a crown which is the visible part used to chew food. The dental implant is made of titanium – the same material used by surgeons for artificial joints. When you lose a tooth, you lose both the root and the crown. To replace the tooth, the surgeon first replaces the root with a small dental implant. Your dentist or prosthodontist will then replace the crown which is usually of a porcelain or Zirconium material.
Time is allowed for bone to heal and grow around the dental implant. The bone bonds with the titanium, creating a strong foundation for artificial teeth. A support post (abutment) is then placed on the implant and a new replacement tooth (crown) is placed on top of the abutment. In many cases a temporary replacement tooth can be attached to the implant immediately after it is placed. If all of your teeth are missing, a variety of treatment options are available to support the replacement teeth.
Dental Implant treatment is a team effort between an oral and maxillofacial surgeon and a restorative dentist. Dr Joseph performs the actual implant surgery, initial tooth extractions, and bone grafting if necessary. The restorative dentist (your dentist) fits and makes the permanent prosthesis. Your dentist will also make any temporary prosthesis needed during the implant process.
Bone Grafting
Minor Bone Grafting
Missing teeth over a period of time can cause your jawbone to atrophy, or resorb. This often results in poor quality and quantity of bone suitable for the placement of dental implants as well as long-term shifting of remaining teeth and changes to facial structure. Most patients, in these situations, are not candidates for dental implants.
Fortunately, today we have the ability to grow bone where it is needed. This not only gives us the opportunity to place implants of proper length and width, but it also gives us a chance to restore functionality and aesthetic appearance.
Minor bone grafting performed in the office can repair the jawbone with inadequate bone structure due to previous extractions, gum disease, or injuries. The bone is either obtained from a tissue bank or your own bone is taken from the jaw. Sinus bone grafts can also be performed to replace lost or inadequate bone in the upper jaw. In addition, special membranes may be used that dissolve under the gum to protect the bone graft and will encourage bone regeneration. This is called guided bone regeneration, or guided tissue regeneration.
Major Bone Grafting
Major bone grafts are typically performed to repair defects of the jaws that may arise as a result of traumatic injuries, tumor surgery, or congenital defects. Large defects are repaired using the patient’s own bone. This bone is harvested from a number of different areas depending on the size needed. The skull (cranium), hip (iliac crest), are common donor sites. These procedures are routinely performed in an operating room and require a hospital stay.
Platelet Rich Plasma
Platelet-rich plasma (PRP) is a by-product of blood (plasma) that is rich in platelets. Until now, its use has been confined to the hospital setting. This was due mainly to the cost of separating the platelets from the blood and a large amount of blood needed to produce a suitable quantity of platelets. New technology permits doctors to perform the same procedure in the office harvesting a sufficient quantity of platelets from a small amount of their own blood. This is drawn from the patient while they are having outpatient surgery.
Why all the excitement about PRP?
PRP permits the body to take advantage of the normal healing pathways at a greatly accelerated rate. During the healing process, the body rushes many cells and cell types to the wound in order to initiate the healing process. One of those cell types is platelets. Platelets perform many functions, including the formation of a blood clot and the release of growth factors (GF) into the wound. Growth factors include platelet-derived growth factors (PDGF), transforming growth factor Beta (TGF), and insulin-like growth factor (ILGF). These function to assist the body in repairing itself by stimulating stem cells to regenerate new tissue. The more growth factors released into the wound, the more stem cells are stimulated to produce new tissue. Thus, PRP permits the body to heal faster and more efficiently.
PRP Has Many Clinical Applications
PRP can be used to aid bone grafting for dental implants. This includes onlay and inlay grafts, Sinus lift grafts, ridge augmentation, closure of the cleft lip, and palate defects. It can also assist in the repair of bone defects created by the removal of teeth, or small cysts and the repair of fistulas between the sinus cavity and mouth.
PRP Also Has Many Advantages
• Safety: PRP is a by-product of the patient’s own blood, therefore, disease transmission is not an issue.
• Convenience: PRP can be generated in the doctor’s office while the patient is undergoing an outpatient surgical procedure such as the placement of dental implants.
• Faster healing: The saturation of the wound with PRP, and growth factors, produces an increase in tissue synthesis and faster tissue regeneration.
• Cost effectiveness: Since PRP harvesting is done in the doctor’s office; the patient does not incur the expense of the harvesting procedure in the hospital or at a blood bank.
• Ease of use: PRP is easy to handle and actually improves the ease of application of bone substitute materials and bone grafting products by making them more gel-like.
Frequently Asked Questions About PRP
Is PRP safe? Yes. During the outpatient surgical procedure, a small amount of your own blood is drawn. The blood is then placed in the PRP centrifuge machine and spun down. In less than 15 minutes, the PRP is formed and ready to use.
Should PRP be used in all bone-grafting cases? Not always. In some cases, there is no need for PRP. However, in the majority of cases, the application of PRP to the bone graft will increase the final amount of bone present, in addition to making the wound heal faster and more efficiently.
Will my insurance cover the costs? No. The PRP application (approximately $400) is paid by the patient.
Can PRP be used alone to stimulate bone formation? No. PRP must be mixed with either the patient’s own bone, a bone substitute material such as freeze-dried bone, or a synthetic bone product.